Quotation of the Day: On Work and Mortality posted first on http://drugsscreeningpage.blogspot.com/ via Blogger Quotation of the Day: On Work and Mortality
0 Comments
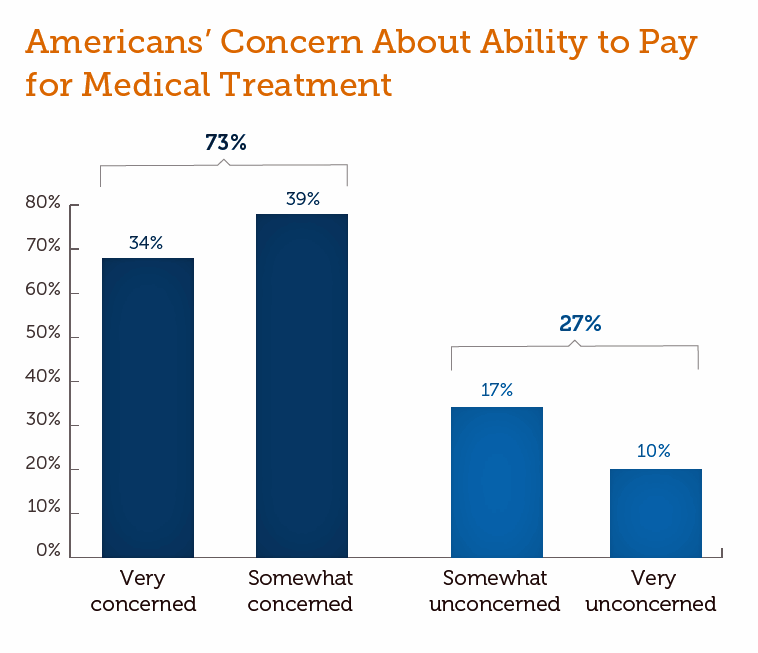
While Costs Are A Top Concern Among Most U.S. Patients So Are Challenges of Poverty Food and Housing10/31/2019 Rising health care costs continue to concern most Americans, with one in two people believing they’re one sickness away from getting into financial trouble, according to the 2019 Survey of America’s Patients conducted for The Physicians Foundation.
In addition to paying for “my” medical bills, most people in the U.S. also say that income inequality and inadequate social services significantly contribute to high medical spending for every health citizen in the nation. The Physicians Foundation conducts this study into Americans’ views on the U.S. health care system every other year. This year’s poll was conducted in September 2019 and included input from 2,001 U.S. adults ages 27-75 who had seen the same doctor at least once in the past year. Digging into the health care cost concerns, the Foundation asked people about their health care affordability cost thresholds — that is, their ability to pay medical bills for an unexpected illness before they hit a personal financial crisis. 42% of Americans could afford a bill of $500 or less before they would have financial issues; 22% could afford between $501 and $2,500; and, 37% could afford more than $2,500 to pay for an unexpected health issue. Cost was ranked as the top issue negatively impacting patient care in this survey, identified by 86% of U.S. health care consumers, followed by waiting for insurance pre-approvals (cited by 72%), using pre-determined treatments based on scientific evidence of similar cases (aka protocols or clinical guidelines (noted by 50% of consumers), and electronic health records (among 30% of people). Related to costs, consumers were asked about factors they believe drive up health care spending. Three-quarters of Americans believe that hospitals, clinics and physicians should look beyond patients medical/clinical needs into root causes like access to healthy food, transportation, and safe/clean housing — the social determinants of health. The study also addressed the politics of health care leading up to the 2020 Presidential election. Cost concerns are playing into peoples’ perspectives on health care reform proposals, with a majority of survey respondents saying they’d be more likely to vote for a candidate that would support expanding private health insurance reforms versus scrapping commercial insurance for a Medicare for All proposal. While a “single payer health care system” was favored by 41% in terms of a candidate’s position, 77% of people could not agree on a definition for what “single payer” means in a U.S. health care system model.
“Average mentions of government have been on the rise since 2017,” Gallup noted in a growing polarized political climate in the U.S. So whose job is it anyway to bolster social, economic and environmental health for a nation’s health citizens? There’s a trend in 2019 which will continue through 2020 where private sector health care providers, Foundations and other non-public sector entities have begun to address social determinants of health. Kaiser Permanente is building a data platform with Unite US to manage and address the challenge, as well as investing in housing for residents in its communities, part of the organization’s $200 mm Thriving Communities Fund.
I laud these programs initiated by private sector businesses and health care stakeholders. Health consumers absolutely want to engage across all industry segments for health, we learned from the Edelman Health Engagement Barometer back in 2010 (shown in the bar chart here taken from my book HealthConsuming). But as we consider our larger personal health ecosystem’s beyond healthcare system touch points, the public sector plays an over-arching role in fundamental public health pillars like infrastructure (think: clean air, clean water), education and food policy. A new study from a global research team published in the Proceedings of the National Academy of Science (PNAS) looked into social, demographic, and economic correlates of food and chemical consumption finding a direct statistical relationship between wastewater and socioeconomic factors: that is, people in lower socioeconomic strata had greater exposure to environmental hazards. These are social determinants of health that lie well beyond the prescription pads of doctors, nurses, pharmacists and disease managers. In tomorrow’s Health Populi blog, I’ll cover specific aspects in the Physicians Foundation 2019 survey addressing prescription drug costs. The post While Costs Are A Top Concern Among Most U.S. Patients, So Are Challenges of Poverty, Food, and Housing appeared first on HealthPopuli.com. While Costs Are A Top Concern Among Most U.S. Patients, So Are Challenges of Poverty, Food, and Housing posted first on http://drugsscreeningpage.blogspot.com/ via Blogger While Costs Are A Top Concern Among Most U.S. Patients, So Are Challenges of Poverty, Food, and Housing When should you schedule an appointment with your doctor or dentist? I had always thought that being one of the first appointments of the day was beneficial because the doctor’s aren’t yet tired from a long day of work. For instance, I try to schedule my dentist appointments early in the morning just for this reason (and because if I go early, it doesn’t much interrupt my work day). However, is there any evidence that earlier appointments lead to better outcomes? A paper by Persson et al. (2019) aim to answer this question by looking at patient appointments and surgeon’s decision to operate. Using Swedish registry data from an orthopedic clinic, the authors find that:
The authors claim this study provides evidence of decision fatigue. After a long day of blogging, however, I’m too tired to determine if this really is or is not decision fatigue. Source:
Physician Decision Fatigue posted first on http://drugsscreeningpage.blogspot.com/ via Blogger Physician Decision Fatigue
…and the NBA season has started! Friday Links posted first on http://drugsscreeningpage.blogspot.com/ via Blogger Friday Links A Health Future with Lyft and Uber as Patient Data Stewards: Rock Healths 2019 Consumer Survey10/29/2019
Rock Health’s Digital Health Consumer Adoption Report for 2019 was developed in collaboration with the Stanford Medicine Center for Digital Health. Rock Health’s research has tracked peoples’ use of telemedicine, wearable technology, digital health tracking, and online health information since 2015, and the results this round show relative flattening of adoption across these various tools. Rock Health’s top-line findings were that:
Start with tracking: nearly 80% of people tracked at least one health metric in 2019, but nearly one-half of that tracking was done in an analog, not digital way. This was a deja vu data point for me, thinking back to Susannah Fox’s study at the Pew Research Group back in 2013 which learned that most people tracked health data “in their heads.”
What do health trackers track, then? The second chart (Figure 3 in Rock Health’s report) illustrates the most popular consumer-tracked health metrics by health conditions of obesity, diabetes, heart disease and hypertension. Note that the darkest green tone identifies the data for tracking via digital methods. Overall, the most common digitally-tracked metric is blood pressure, followed by weight. The most digitized tracking was for blood sugar among people managing diabetes, at 29% of patients, followed by 24% of people tracking blood pressure digitally among people with hypertension as well as heart disease, and 23% of people dealing with obesity tracking weight digitally. Only about 20% of people who tracked a health metric shared that data with a health care provider, Rock Health learned. Among consumers willing to share health information, the most trusted touch point is “my physician,” with whom 86% of people said they’d share in 2017 but dropping to 73% in 2019. Second in sharing-line were “my health insurance company” and “my pharmacy” for just over one-half of consumers, a percentage which stayed fairly flat between 2017 and 2019. The proportion of people willing to share data with research institutions fell by 44% to 34% in the two years, and with health tech companies, flat at 23% between 2018-2019. Only one in five consumers would be willing to share their data directly with pharma companies, to Rock Health’s third point about willingness-to-share-with-whom.
Health Populi’s Hot Points: The third chart shown here, Figure 9 from the Rock Health report, presents data on the tech companies with whom U.S. consumers would be most willing to share their health data. This information compelled me to return to the previous responses to this question in Rock Health’s surveys starting back in the 2015 study into digital health consumer adoption. In 2015, Google was still the top company with whom people would share data — at a percent of 10.2% of total consumers, followed by:
You will quickly say, “ah! The proportion of consumers willing to share personal health information with pure-play tech companies has grown exponentially!” True — yet the proportions have dropped between 2018 and 2019 as follows:
And this year, Rock Health added in Uber and Lyft, with whom 22% and 16% of consumers would share health data, respectively. We see the continued evolution of health-data ecosystems, as well as the re-definitions of what a “tech company” is vis-a-vis a “health-tech company.” Clearly, with the rumors this week that Google may be looking to acquire Fitbit, Google Health would continue to grow its data mine massively through that transaction. And, as Cerner announced its collaboration with Uber Health this week, we see a health IT company expanding beyond what an EHR could be. The post A Health Future with Lyft and Uber as Patient Data Stewards: Rock Health’s 2019 Consumer Survey appeared first on HealthPopuli.com. A Health Future with Lyft and Uber as Patient Data Stewards: Rock Health’s 2019 Consumer Survey posted first on http://drugsscreeningpage.blogspot.com/ via Blogger A Health Future with Lyft and Uber as Patient Data Stewards: Rock Health’s 2019 Consumer Survey
Quotation of the Day: On Work and Mortality posted first on http://drugsscreeningpage.blogspot.com/ via Blogger Quotation of the Day: On Work and Mortality While Costs Are A Top Concern Among Most U.S. Patients So Are Challenges of Poverty Food and Housing10/28/2019 Rising health care costs continue to concern most Americans, with one in two people believing they’re one sickness away from getting into financial trouble, according to the 2019 Survey of America’s Patients conducted for The Physicians Foundation.
In addition to paying for “my” medical bills, most people in the U.S. also say that income inequality and inadequate social services significantly contribute to high medical spending for every health citizen in the nation. The Physicians Foundation conducts this study into Americans’ views on the U.S. health care system every other year. This year’s poll was conducted in September 2019 and included input from 2,001 U.S. adults ages 27-75 who had seen the same doctor at least once in the past year. Digging into the health care cost concerns, the Foundation asked people about their health care affordability cost thresholds — that is, their ability to pay medical bills for an unexpected illness before they hit a personal financial crisis. 42% of Americans could afford a bill of $500 or less before they would have financial issues; 22% could afford between $501 and $2,500; and, 37% could afford more than $2,500 to pay for an unexpected health issue. Cost was ranked as the top issue negatively impacting patient care in this survey, identified by 86% of U.S. health care consumers, followed by waiting for insurance pre-approvals (cited by 72%), using pre-determined treatments based on scientific evidence of similar cases (aka protocols or clinical guidelines (noted by 50% of consumers), and electronic health records (among 30% of people). Related to costs, consumers were asked about factors they believe drive up health care spending. Three-quarters of Americans believe that hospitals, clinics and physicians should look beyond patients medical/clinical needs into root causes like access to healthy food, transportation, and safe/clean housing — the social determinants of health. The study also addressed the politics of health care leading up to the 2020 Presidential election. Cost concerns are playing into peoples’ perspectives on health care reform proposals, with a majority of survey respondents saying they’d be more likely to vote for a candidate that would support expanding private health insurance reforms versus scrapping commercial insurance for a Medicare for All proposal. While a “single payer health care system” was favored by 41% in terms of a candidate’s position, 77% of people could not agree on a definition for what “single payer” means in a U.S. health care system model.
“Average mentions of government have been on the rise since 2017,” Gallup noted in a growing polarized political climate in the U.S. So whose job is it anyway to bolster social, economic and environmental health for a nation’s health citizens? There’s a trend in 2019 which will continue through 2020 where private sector health care providers, Foundations and other non-public sector entities have begun to address social determinants of health. Kaiser Permanente is building a data platform with Unite US to manage and address the challenge, as well as investing in housing for residents in its communities, part of the organization’s $200 mm Thriving Communities Fund.
I laud these programs initiated by private sector businesses and health care stakeholders. Health consumers absolutely want to engage across all industry segments for health, we learned from the Edelman Health Engagement Barometer back in 2010 (shown in the bar chart here taken from my book HealthConsuming). But as we consider our larger personal health ecosystem’s beyond healthcare system touch points, the public sector plays an over-arching role in fundamental public health pillars like infrastructure (think: clean air, clean water), education and food policy. A new study from a global research team published in the Proceedings of the National Academy of Science (PNAS) looked into social, demographic, and economic correlates of food and chemical consumption finding a direct statistical relationship between wastewater and socioeconomic factors: that is, people in lower socioeconomic strata had greater exposure to environmental hazards. These are social determinants of health that lie well beyond the prescription pads of doctors, nurses, pharmacists and disease managers. In tomorrow’s Health Populi blog, I’ll cover specific aspects in the Physicians Foundation 2019 survey addressing prescription drug costs. The post While Costs Are A Top Concern Among Most U.S. Patients, So Are Challenges of Poverty, Food, and Housing appeared first on HealthPopuli.com. While Costs Are A Top Concern Among Most U.S. Patients, So Are Challenges of Poverty, Food, and Housing posted first on http://drugsscreeningpage.blogspot.com/ via Blogger While Costs Are A Top Concern Among Most U.S. Patients, So Are Challenges of Poverty, Food, and Housing
…and the NBA season has started! Friday Links posted first on http://drugsscreeningpage.blogspot.com/ via Blogger Friday Links Health and our health information are deeply personal. Changing health care and inspiring positive health behaviors is hard to do.
But we must and we will, a group of inspiring and inspired people who work across the health/care ecosystem affirmed this week in Dallas at the conference of Medecision Liberation 2019. I was engaged at this conference to wear several hats — as a keynote speaker, a sort of “emcee,” and, finally, to trend-weave the many talks and discussions happening throughout the meeting. This post is my synthesis of the summary I delivered live at the end of the conference, which one of the attendees described as “poetry slam-meets-healthcare.” I quite like that new-and-improved Cliff’s Notes metaphor. Deb Gage, Medecision CEO, kicked off the meeting. The inspiration started within minutes as Deb shared several personal stories involving the health care system and its flaws. Think of Deb as the proverbial shoe-maker’s child with no shoes: she leads a company helping drive digital transformation in health care, but two people she loved, and she herself, had all been failed by some aspect of fragmented health care delivery in America.
Her learning, and ours: “We don’t need new tech….we need a single person view.” Furthermore, Deb pointed to this quote from Dr. Atul Gawande — that our job is not to ensure health and survival…it’s to enable well-being. This ethos echoed throughout the 36 hours of Liberation 2019, culminating with the mantra of Nick Adkins, Co-Founder of the #PinkSocks Life community, who challenged us to look each other in the eye in close personal space to a new acquaintance and say (and mean), “I see you.”
My own talk on the acronym I coined for this event, “TiSH,” spoke to each of our challenges with Trust, Stress, and Health Literacy. Taken together, these can be a toxic cocktail when not aligned for positive health behavior. Stress in America today crosses socioeconomic strata when it comes to health care costs several research studies have found that I cited, including surveys from the American Psychological Association and the Kaiser Family Foundation. The call-to-action Rx for this is to get to know a patient’s values in terms of the life-flows and personal goals, as well as their “value” for health care — the ability and willingness to pay, their personal definition of affordability, and how that plays into their potential or actual self-rationing behavior due to cost. As many as 1 in 2 Americans has avoided some aspect of health care due to cost in the past year, such as postponing a needed visit to a doctor or not filling a prescription drug.
During Liberation 2019, there were many moments of inspiration, but none more visceral or personal than the family history shared by Gary Mendell, founder of Shatterproof. Gary’s son was addicted to opioids and ultimately, after many months of being clean, took his own life. Gary’s mission with Shatterproof has four pillars, none more important than de-stigmatizing mental health and especially addiction by recognizing that it’s a legitimate healthcare condition worthy of parity of treatment priority and payment just like physical conditions such as cancer or heart disease.
From Gary and the challenge of addiction, we moved and were moved by Dr. Shoshana Ungerleider’s leadership of Endwell, an organization devoted to expanding the concept of a good death. The U.S. fails in this end-of-life patient and family experience, and so many of us in the room where Shoshana shared her mission-driven message nodded, teased up, shook our heads, and stared this truth in its face. In Shoshana’s introductory video, a doctor from Stanford said, “Coming here (to the Endwell meet-up) and dealing with end of life makes me proud to be part of health care.” There’s nothing more personal than one’s own death, and Shoshana challenges the siloed health care system to break down the siloed of home care, hospice, inpatient care, physician care, faith-based organizations, and disease advocacy groups to come together for the benefit of streamlining and humanizing death to make it just as enlightened a patient experience as other aspects of health care on life’s continuum.
Julie Murchinson, CEO of Health Evolution, concluded the meeting with her insights into “tribes.” She noted that each of us, within and outside of health care, but each of us people is a member of a tribe that’s unique to us, riffing on the work of Dave Logan. Some of us are in tribes where we feel we’re great (and “you’re not”). Some of us are in tribes where we feel marginalized by society and hang with other people in our tribes who feel the same way. Some of us feel communal in our tribe in that our operating system is inclusive for the whole versus the individual in and of ourselves. Recognizing that we are all in tribes, sometimes quite different than the ones with which we identify.
She pointed to Greta Thunberg, who at 16 has indeed inspired a movement to popularize climate change across borders, age groups, social strata, and political persuasions. Greta is as good an inspirational role model as any we can channel in these cynical days. That’s liberating. That’s Liberation 2019. Thank you, Medecision team, for convening this exciting, inspiring, informative meeting. This isn’t my job at moments like this; it’s a mission. The post Making Health Care Better, from the N of 1 to the Public’s Health – Trend-Weaving Medecision Liberation 2019 appeared first on HealthPopuli.com. Making Health Care Better, from the N of 1 to the Public’s Health – Trend-Weaving Medecision Liberation 2019 posted first on http://drugsscreeningpage.blogspot.com/ via Blogger Making Health Care Better, from the N of 1 to the Public’s Health – Trend-Weaving Medecision Liberation 2019 As people age, falls become not only more common, but more problematic. Every year 300,000 elderly Americans are hospitalized for a hip fracture, and 95% of these fractures are due to falls. Falls are the leading cause of fatal and non-fatal injuries among the U.S. elderly. What are people doing about it? Kaiser Health News has two interesting stories on the topic. First, younger elderly individuals are moving to more “Age-proofed” housing:
Baby boomers want a safe place for them to live as they age. While this caution is well-placed, another KHN article argues that hospitals may be too cautious. In an effort to prevent falls, hospitals may be keeping the elderly on bedrest for too long. Kaiser Health News reports:
Part of the reason hospitals are overly cautious is that starting in 2008, the Centers for Medicare and Medicaid Services imposed financial penalties on hospitals whenever patients fell. The penalties increased when the Affordable Care Act was passed. This created a culture where hospital staff were perhaps overly fearful of falls, as CMS only tracks fall rates, not patient mobility at discharge. Preventing falls is important. But physicians and nurses need to be able to use their discretion to help determine to balance the risk from falls against a lack of mobility. Fear of Falling posted first on http://drugsscreeningpage.blogspot.com/ via Blogger Fear of Falling |
Anthony Williams
I am an experienced pharmacist with interest in content writing. I am also a known blogger for Drug Home Health Testing, an online drug testing and home health business. I write mostly about drug tests but many more from this sector will be coming soon. I am also a top selling author of Drug Test Dilemma! I have previously run a membership site for Drug home test making it in the most convenient way and the same knowledge has been compiled to create my new project Drug Test Dilemma. Personal Links |
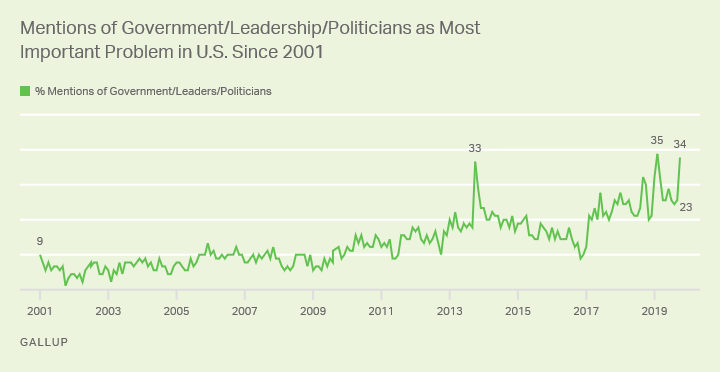 Health Populi’s Hot Points: Americans’ mentions of “government” as a top U.S. problem are near a record high,
Health Populi’s Hot Points: Americans’ mentions of “government” as a top U.S. problem are near a record high, 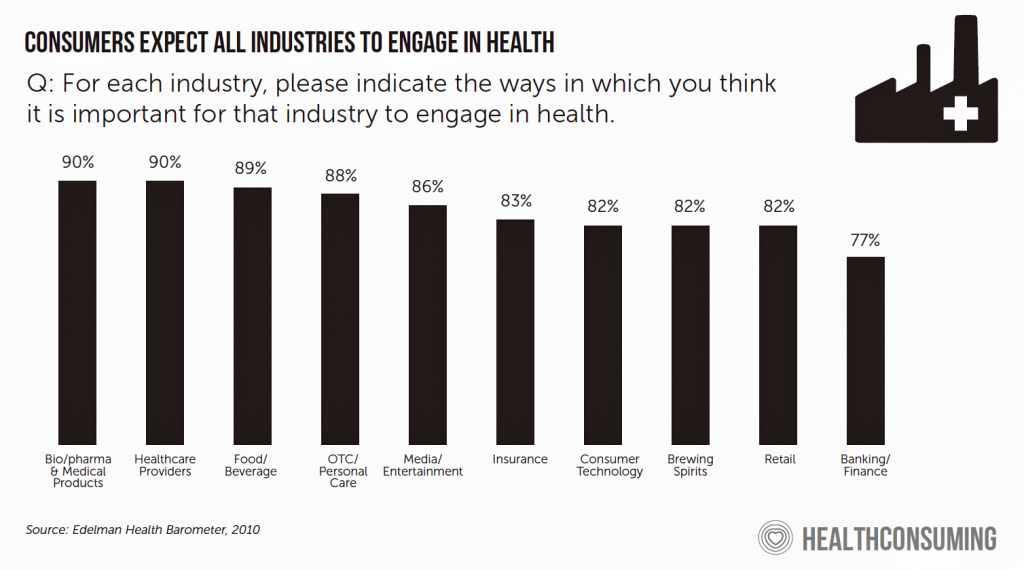 Microsoft recently launched a program to build housing for people around its Seattle headquarters. Microsoft is working with Humana on how to leverage data to help people age in place safely and health-fully. Humana connects with consumers on issues of loneliness and mental health through its campaign with spokespeople Nick Jonas, Queen Latifah and Ted Danson. Humana also launched a “Bold Goal” initiative to boost healthy food access for people enrolled in the plan’s Medicare Advantage programs.
Microsoft recently launched a program to build housing for people around its Seattle headquarters. Microsoft is working with Humana on how to leverage data to help people age in place safely and health-fully. Humana connects with consumers on issues of loneliness and mental health through its campaign with spokespeople Nick Jonas, Queen Latifah and Ted Danson. Humana also launched a “Bold Goal” initiative to boost healthy food access for people enrolled in the plan’s Medicare Advantage programs.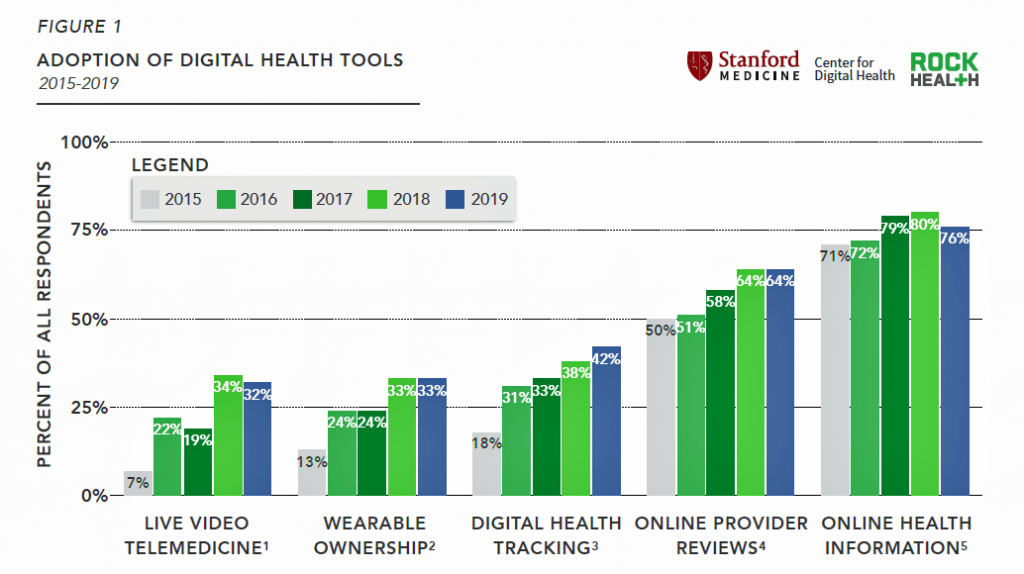 Patients searching online for health information and health care provider reviews is mainstream in 2019. Digital health tracking is now adopted by 4 in 10 U.S. consumers.
Patients searching online for health information and health care provider reviews is mainstream in 2019. Digital health tracking is now adopted by 4 in 10 U.S. consumers.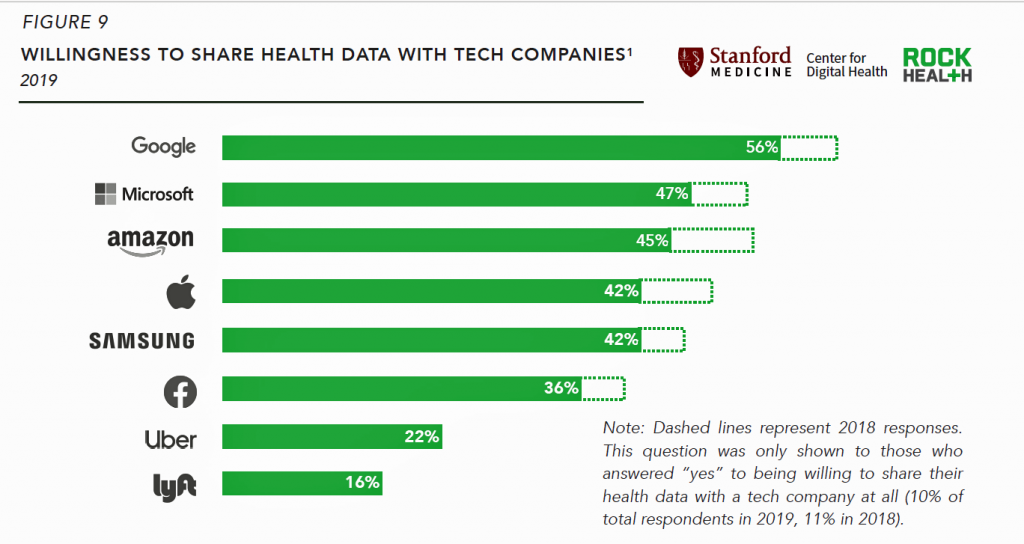

 Deb shared the experiences of Sam, her friend of 25 years, who had the quite-typical co-morbidity of multiple chronic physical conditions baked with mental health issues. Deb’s Dad, Ray, having lost his wife (Deb’s mom), was living alone, aging with some common conditions that come with living long and well, and wanting to stay independent in a health-and-social environment that doesn’t make this so easy to do. And Deb herself, surviving a tough condition, found that her own medical records were located in four disparate health systems based on the fragmented nature of her care delivered through different provider organizations.
Deb shared the experiences of Sam, her friend of 25 years, who had the quite-typical co-morbidity of multiple chronic physical conditions baked with mental health issues. Deb’s Dad, Ray, having lost his wife (Deb’s mom), was living alone, aging with some common conditions that come with living long and well, and wanting to stay independent in a health-and-social environment that doesn’t make this so easy to do. And Deb herself, surviving a tough condition, found that her own medical records were located in four disparate health systems based on the fragmented nature of her care delivered through different provider organizations.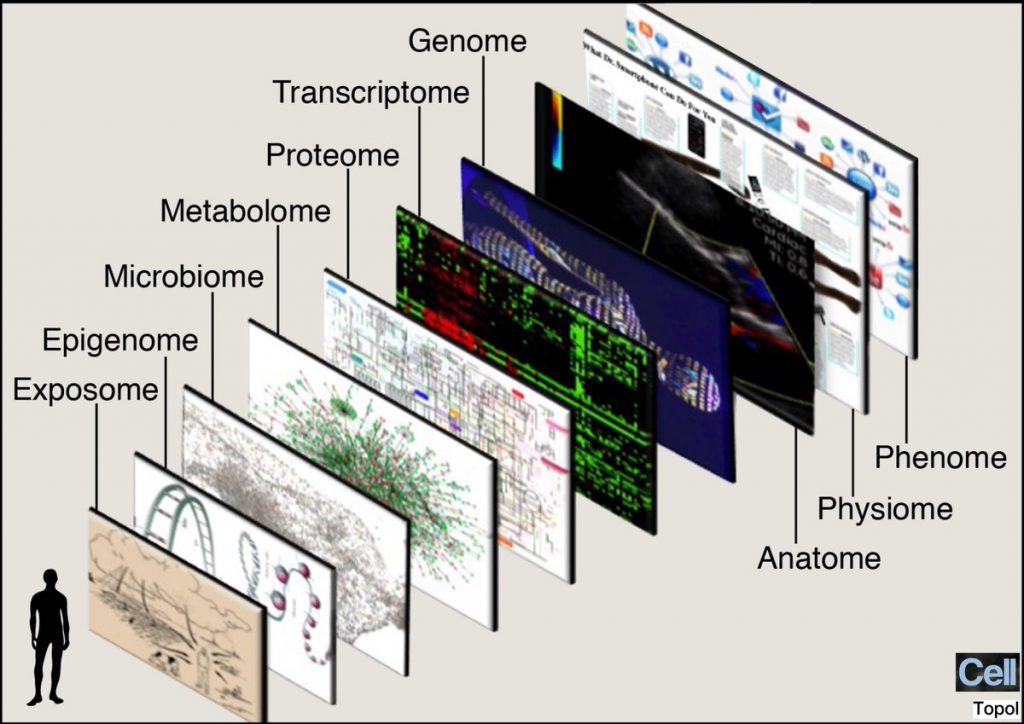 Another riff on “I see you,” that N of 1 person-patient-consumer, was Dr. Eric Topol’s explicit mission for Deep Medicine: that is, to personalize treatment based on evidence, not on the long-accepted
Another riff on “I see you,” that N of 1 person-patient-consumer, was Dr. Eric Topol’s explicit mission for Deep Medicine: that is, to personalize treatment based on evidence, not on the long-accepted So we’ve spoken to the N of 1 patient-person and the N of 1 physician-clinician. But if we want to change health care for the better, we must look into the eyes, Nick Adkins-style, of workers in health care. Chris Mahai, who runs Aveus, Medecision’s consulting division, wrote the book
So we’ve spoken to the N of 1 patient-person and the N of 1 physician-clinician. But if we want to change health care for the better, we must look into the eyes, Nick Adkins-style, of workers in health care. Chris Mahai, who runs Aveus, Medecision’s consulting division, wrote the book  Gary talked of a vision, “that our society would look this straight in the eye, prevent, treat with love and empathy and with programs based on science.” This vision weaves together elements shared in the conference by all of the speakers, with Gary’s family’s learning this in the most personal, devastating way.
Gary talked of a vision, “that our society would look this straight in the eye, prevent, treat with love and empathy and with programs based on science.” This vision weaves together elements shared in the conference by all of the speakers, with Gary’s family’s learning this in the most personal, devastating way.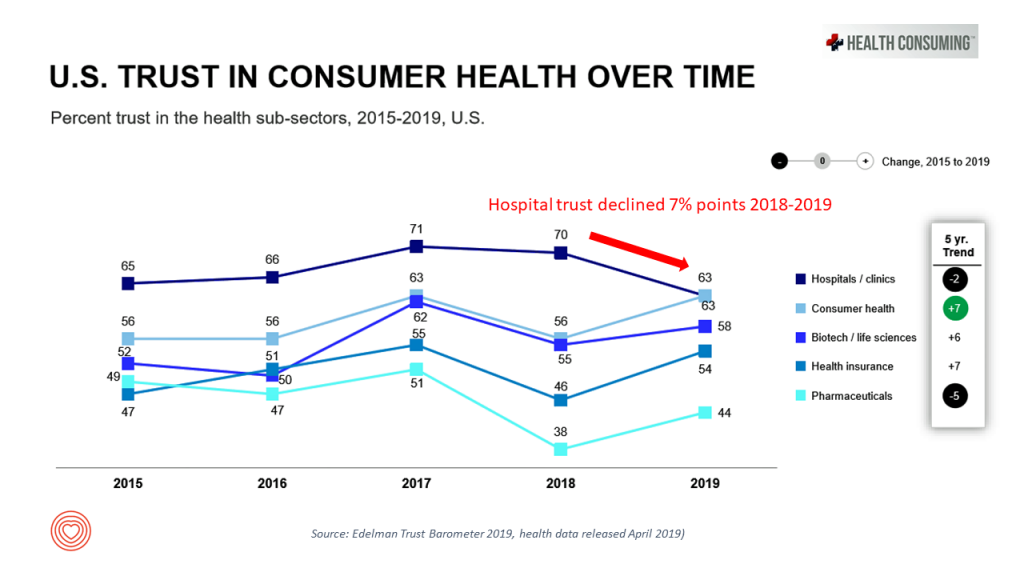 Patients and families who have felt betrayed by the health care system, as Gary and many of Shoshana’s communities, may have reacted, must feel trust again with those segments of the health/care ecosystem from whom they are alienated. Trust is a precursor for health engagement, and Lynn Hanessian and Cydney Roach of Edelman did a deep dive into the
Patients and families who have felt betrayed by the health care system, as Gary and many of Shoshana’s communities, may have reacted, must feel trust again with those segments of the health/care ecosystem from whom they are alienated. Trust is a precursor for health engagement, and Lynn Hanessian and Cydney Roach of Edelman did a deep dive into the 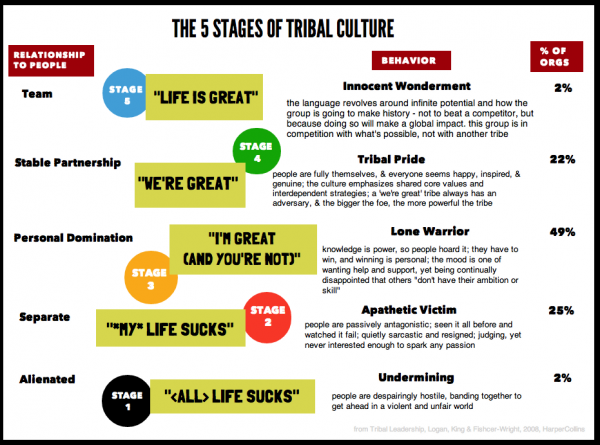 Julie’s call-to-action asked each and all of us: “How do we drive change in health care as a tribe to make a movement?”
Julie’s call-to-action asked each and all of us: “How do we drive change in health care as a tribe to make a movement?” RSS Feed
RSS Feed
